The U.S. Food and Drug Administration receives over 100,000 yearly reports about suspected medication errors. Worse yet, an estimated 7,000–9,000 people die annually in the U.S. due to such mistakes. While handwritten prescriptions aren't solely to blame, changes to the current prescription process could help address this widespread problem.
Handwritten prescriptions are outdated and inconvenient for everyone in healthcare. Fortunately, e-prescribing software offers a solution, whether used as a standalone application or integrated into an Electronic Health Record (EHR) or Electronic Medical Record (EMR) system. E-prescriptions travel accurately, rapidly, and seamlessly from doctor to pharmacist to hospital administration to insurer.
In this article, we walk you through the main things you need to know about e-prescription software. We discuss key market players, must-have features, possible development challenges, and monetization models. Let’s start.
What Is E-Prescribing Software?
Before diving deep into the details, let’s briefly remind you what e-prescribing software, also termed e-Rx, is. Simply put, it’s a form of telehealth that allows sending prescriptions electronically from the doctor's office to the pharmacy. Once the pharmacy receives the digital prescription, they can fill the medication order immediately. In this way, e-prescribing software eliminates the need for calls or emails. So the patients can enjoy the simplicity and progressiveness of the solution.
According to the Center for Connected Health Policy, clinicians can prescribe most medications via telehealth. However, there are minor differences between state and federal regulations regarding the appropriate use of technology for prescribing. For example, most states don't allow establishing a patient-provider relationship solely through emailed questionnaires, faxes, or messages.
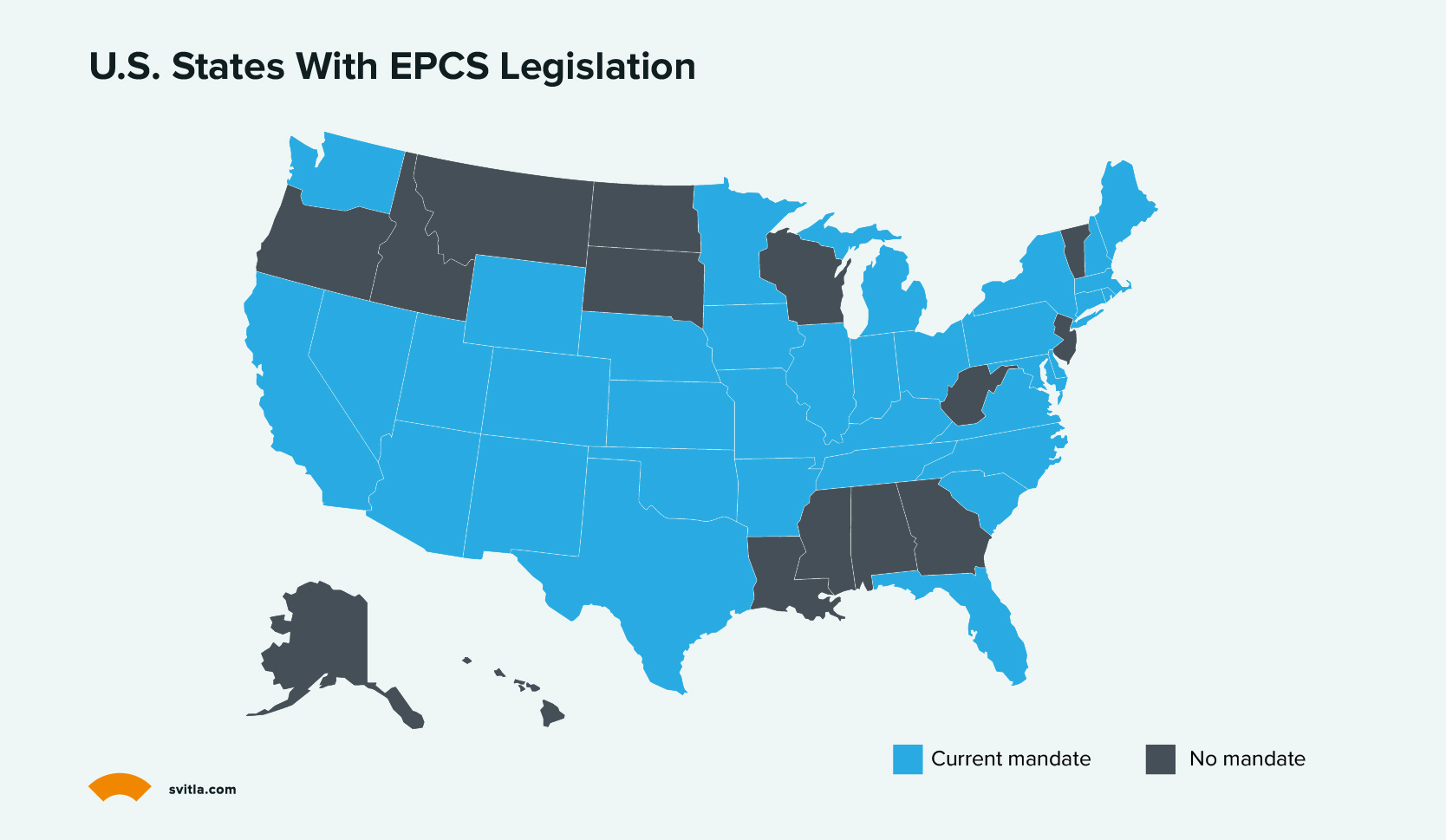
As e-prescribing advances, electronically prescribing controlled substances (EPCS) grows increasingly vital. EPCS compliance necessitates third-party audits confirming that e-prescribing software satisfies U.S. Drug Enforcement Agency standards. Notably, before e-prescribing controlled substances, most states mandate a patient examination, in-person or via telehealth. Though, policies differ — some states treat in-person and telehealth exams equally regarding this requirement.
How E-Prescribing Software Works
E-prescribing software allows physicians to write and send prescriptions electronically to pharmacies instead of traditional paper scripts. This is achieved via cloud-based platforms that doctors can access remotely through web dashboards on desktop computers or mobile devices like tablets and smartphones. The accessibility empowers doctors to prescribe medications from any location with internet connectivity.
To begin the e-prescribing process, physicians use the integrated software to look up the patient’s health plan and medication history information while meeting with them. This background helps inform prescription decisions. Doctors can see which drugs are covered favorably under the patient’s insurance plan. Once the doctor finalizes the prescription details within the software, they hit submit, which electronically transmits the prescribed medication directly to the preferred pharmacy selected by the patient. This prompt electronic delivery enables faster fulfillment, so prescriptions are ready sooner for patient pickup. The software also includes workflows to facilitate prescription renewals and refills electronically between doctors and pharmacies.
Benefits of E-Prescription Software
The primary goal of digital prescription solutions is to improve prescription safety and reliability. But they offer other meaningful benefits, too:
- Reduced pharmacist errors. E-prescriptions are extremely clear about treatment and dosage, requiring less interpretation by the pharmacist. This can decrease prescription mistakes, ensuring patients have accurate information on how to take a drug. Studies show that e-prescribing can reduce medication errors by 35%.
- Instant clinical alerts. Over 4.5 million ER/doctor visits annually stem from preventable adverse drug events. E-prescription systems can interface with electronic records to alert clinicians about allergy risks, drug interactions, high dosages, etc. They also catch duplicate therapies.
- Prescription fulfillment tracking. E-prescribing lets doctors know which patients have filled/refilled medications. This helps ensure treatment compliance and reduces hospital readmissions.
- Increased efficiency. Handwriting scripts is tedious and inefficient. E-prescribing allows mass renewals and quick emergency refills when needed.
- Fewer readmissions. Hospital readmissions are reduced by 13% by catching inappropriate prescriptions. By accessing patient allergy/history data, e-prescribing prevents errors and dangerous interactions.
- Major cost savings. Through better outcomes, efficiency gains, and fewer patient visits, e-prescribing has saved $140-$240 billion over the past decade. As the technology improves, the savings could increase further.
Key Market Players
Now, that we’ve discussed the basics, let’s overview the most prominent market players. So, you can find fresh ideas for your future project and get inspired.

RXNT
It’s an end-to-end cloud platform that centralizes real-time patient health and prescription data at the point of care for informed decision-making. RXNT simplifies workflow efficiency through intuitive EPCS-certified e-prescribing tools, two-way pharmacy integrations, scheduling coordination, and billing or referral processing. The system is fully customizable across module functionality and user permissions to match practice needs.
Patients access a personalized portal with prescription management, lab results, telehealth services, and self-scheduling. This level of connectivity and transparency promotes better health outcomes.
Price: from $665 per year
CharmHealth
CharmHealth simplifies practice management through an integrated care coordination platform accessible anywhere via a web browser or mobile app. Core features like billing, scheduling, and robust e-prescribing capabilities allow providers to optimize workflows.
The software connects to over 70,000 pharmacies to transmit and track prescriptions electronically. Streamlined refill approvals further reduce administrative workload. The app ensures usability and patient data protection through HIPAA-compliant design.
Price: from $350 per provider per month
Kareo Clinical
Kareo Clinical is a user-friendly EHR system accessible via the web, iPad, iPhone, and Apple Watch. The software simplifies patient record management and workflows for independent general practices.
Kareo enables comprehensive e-prescribing through partnerships that tap into real-time prescription data and expansive pharmacy networks. This allows the platform to focus entirely on customer needs rather than building infrastructure. Custom documentation templates also prevent restrictive one-size-fits-all approaches. The streamlined functionality suits independent practitioners well but lacks robust tools for niche specialties.
Price: Not disclosed
Elation Health
Elation Health offers the primary care experience through user-centric design. The web and mobile EHR platform balances robust features with intuitive workflows to enable personalized care plans. While covering standard functionality like e-prescribing, billing, and patient charting, Elation Health further streamlines medication management. Capabilities like prescription renewal or cancellation and SMS messaging drive efficiency.
The system also provides unique support for membership and concierge practices. Tools facilitating recurring payments align well with emerging care models focused on prevention versus reactive treatment.
Price: $275 per month (billed annually)
Benchmark Systems
Benchmark Systems adapts to the unique needs of specialty providers through flexible deployment options and modular EHR tools. The web, desktop, and mobile platform covers everything from e-prescribing to documentation with configurability to match specialty-specific workflows.
Benchmark enables specialty clinics to augment core functionality like billing with customized templates, protocols, and trackers unique to the populations served. This prevents reliance on general practice models lacking the nuance required for quality specialty care. Benchmark Systems allows robust platform modification down to the workflow for specialty providers seeking an adaptable solution without generic constraints. Practices can effectively balance standardization for reporting with specialization for optimal care.
Price: Not disclosed
Essential Features for E-Prescription Apps
To make your e-prescription app successful, you should implement some core features. Here are some of the main ones:
Patient Features
User login. Patients should be able to log in and provide health details like age, gender, and insurance. This allows the capture of critical info upfront.
- Video consultations. Video calls enable patients and doctors to interact in real-time. This functionality is central to e-prescribing apps, letting patients conveniently explain issues.
- Doctor and pharmacy finder. Integrated geolocation and mapping identifies nearby doctors and pharmacies based on patient location. This facilitates urgent needs and quicker fulfillment.
- Doctor reviews. Patients can leave feedback on the doctors’ performance. This feature boosts platform transparency and aids selection for future users.
- Payment processing. Onboard payment systems are necessary for patients to pay consultation fees. Integrated APIs link to payment gateways to enable seamless transactions.

Doctor Features
- Appointment scheduling. Doctors can manage consultations and time slots automatically via calendar integrations. These streamline visit coordination across the patient base.
- Secure messaging. In-app communication tools facilitate the exchange of sensitive patient information like lab reports and prescriptions. Data security is paramount to ensure regulatory guidelines are met.
- Appointment management. Doctors need the capability to accept/reject appointment requests based on schedules. This prevents bottlenecks and unfinished consultations.
- Video conferencing. Video chat platform integration is vital for visual diagnosis and direction. Doctors can better assess symptoms and guide the next steps through face-to-face camera interaction.
- Push notifications. Prompt notifications keep doctors updated on appointment requests and critical patient updates requiring immediate attention. This feature is essential for responsiveness.
- Allergy tracking. The app stores patient allergy data to enable doctors to perform safety checks before prescribing new medications.
- Medication database. The comprehensive catalog of branded and generic drug info allows easy search by parameters like name, class, and specialty.
- Refill request processing. The app lets patients automatically request prescription refills and allows doctors to approve or deny them electronically quickly.
- New prescriptions. The app lets doctors electronically prescribe to in-network pharmacies for new scripts outside refills.
- Prescription cancellation. The functionality allows doctors to cancel existing prescriptions if treatment plans change electronically. Patients can also submit cancellation requests via the app.
- Pending Rx tracking. The dashboard highlights pending medications for patients, so doctors can efficiently prescribe the next required course in a treatment cycle.
- Electronic transmission. Direct integration with pharmacy systems allows doctors to have one-click prescription transmission and status tracking.
- Controlled substances. Special workflows help physicians control patients' usage of substances like opioids. This deters potential misuse and abuse.

Advanced E-Prescription Features
You can also add some extra capabilities. So, your future application will stand out from the competitors.
- Voice search. Patients can verbally search for providers by name instead of typing. This feature improves convenience and platform accessibility.
- Record video sessions. Saved visit recordings allow patients to revisit recommendations and prescribed treatments. This aids in better retention and compliance.
- Medication reminders. Custom notifications can remind patients when to take medications per doctor recommendations. This prevents missed dosages.
- Document management. Secure digital lockers help manage patient records and critical documentation. This gives patients full control over sensitive medical history.
- Document scanning. Integrated scanning improves images of paper documents before digitization and processing. This results in sharp, legible files.

Common Challenges to E-Prescription App Development
Even minor non-compliance with HIPAA rules can result in major financial penalties and reputational damage. Here are key pitfalls to address when developing an advanced telemedicine solution:
- Inappropriate PHI handling. Deleting or copying patient health information outside strict access protocols increases data breach risks, exposing sensitive data to unauthorized parties. Be sure you provide role-based data control instead.
- Uncontrolled system access. Granting universal data access fails to safeguard tests around ethical “minimum necessary” standards. Employees should only interact with relevant patient records.
- Inadequate data retention policies. While ambiguous, HIPAA does require establishing and following clear medical record retention policies in line with local statutes.
- Insufficient patient access. Patients have a right to obtain copies of their records. Ensure straightforward review and export without introducing identity risks.
- Unprotected storage infrastructure. Apply multidimensional security like encryption, access controls, and logs to all storage media, regardless of format. Monitor for suspicious access.
To Conclude
In a nutshell, e-prescription software is a game-changer in healthcare. It tackles medication errors and boosts patient safety by ditching old-fashioned handwritten prescriptions for electronic ones. Big players like RXNT, CharmHealth, Kareo Clinical, Elation Health, and Benchmark Systems bring diverse solutions, like e-prescribing, billing, healthcare management, and telehealth. So, the lives of patients and physicians become easier.
To nail e-prescription app development, you must include must-have features for patients and doctors. Think secure messaging, appointment management, video chats, medication databases, and controlled substance workflows. And don't forget to tackle challenges like HIPAA compliance, data security, and easy patient access. These innovations improve patient safety, save costs, improve efficiency, and make the whole healthcare experience smoother for everyone involved.
Do you want to be ahead of the race? Svitla Systems is here to help you. Contact us to develop an advanced e-prescription application!





